The modern life stages of women are changing everything we know about fertility and parenting.
Female Fertility in 2018: What Every Millennial Needs to Know *Now*

Brooke Wallace*, an archivist librarian, calls me from uptown Manhattan on her lunch break. We’re connecting because she just finished the process of freezing her eggs and I want to know how it went.
We start at the beginning. Wallace tells me she first considered the procedure when she and her long-term boyfriend finally broke up after realizing they couldn’t get past him not wanting children. It was a painful split for the both of them, and when the now-36-year-old finally did begin dating again, she found that her dwindling fertility was putting a lot of pressure on how she was navigating the modern dating landscape.
Ironically it was a man who she had been out with a few times that informed her about Extend Fertility, a relatively new, boutique egg-freezing clinic in New York City that caters to women just like Wallace — professional women who are open to the idea of having kids eventually, just not quite yet.
“The minute I decided I wanted to do it I felt empowered,” Wallace recalls. “It was like something clicked inside me. My fear of needles just went to the side and I was committed to doing it. I went into that first consultation and was like, ‘Sign me up. Let’s schedule this for my next cycle.’”
And she did just that. On October 1, 2017, Wallace had 15 eggs frozen.

We’re in the midst of an unprecedented era in the history of female fertility. Earlier this year, the Centers for Disease Control and Prevention reported that, for the first time ever, American women in their early 30s are having more babies than those in their 20s.
But this shouldn’t come as a huge surprise: At the start of the 2017 fall college term, women were estimated to outnumber men on campuses by 2.6 million. A well-educated, career-focused woman is no longer a rarity; she’s the norm.
Overall, the average age of new moms still hovers around 28, but that number has crept higher and higher in recent decades. The average age of first-time moms was 21 in the 1970s, but by the early 2000s, it was up to 24. The average millennial woman in the US has officially traded the nursery for a seat at a startup.
Despite the strides this generation has made to level out the professional playing field, women are still faced with a biological factor they don’t have much control over: their ovarian reserves. We may be shattering glass ceilings in the workforce, but as author and egg-freezing advocate Agnes Fischer likes to say, ”Our most productive years just happen to coincide with our most reproductive years.” Whether or not there’s adequate science to back that belief up, the fact of the matter is, the necessities of modern life pushing the average age of American childbearing later than ever.
So, I ask in my best Carrie Bradshaw voice: What are women to do?

While biological clocks, unfortunately, cannot be adjusted to reflect the shifted timeframes of contemporary life, when there is a demand in the market, new businesses will inevitably find a way. Case in point: Modern Fertility, a new, at-home fertility test made specifically for ladies like Wallace.
Afton Vechery, who co-founded the company with former UBERHealth exec Carly Leahy in August, explains that she initially became invested in the women’s fertility industry after she decided to get a fertility test done and found herself footing a $1,500 medical bill for it.
“It really stuck with me that infertility today isn’t even treated as a medical condition in a lot of the US,” says Vechery, who had previously worked as a product manager for the genetic testing company 23AndMe. “I started talking to more women and it became this incredibly common theme. Most of us have this really high anxiety about the future and our fertility, but we have no good way to test it.”
Modern Fertility aims to simplify the testing process. Customers receive a testing kit in the mail that asks them to submit a blood sample, which they return in a provided, prepaid envelope to be processed by Modern Fertility’s lab. Within a few days, customers receive a “fertility score,” which is essentially a personalized hormone report plus an age-specific score that they can track over time. The report shows how one user’s ovarian reserve, ovulation, and general body systems compare with others of the same age.
It sounds like a super helpful tool and a first step in the reproductive journey, but here’s the inevitable roadblock: Fertility isn’t a particularly sexy topic. Even the word rolls off the tongue in a kind of jumbled plop. Until it’s something women are seriously considering, fertility isn’t necessarily an issue that’s tactfully explored.
So how do Vechery and Leahy plan to get their target demographic — busy millennial women who might be busy getting doctorate degrees or running businesses — to consider their own fertility as a serious aspect of their overall health? And furthermore, to drop upwards of $150 on a kit?
Vechery is hoping the increasing conversations around the topic will be enough. “We’ve spent a lot of time thinking about this,” she tells me. “Women are talking about it more and more. We did research and found that 86 percent of women in our target demographic [21- to 40-year-olds] have anxiety about their ability to have kids someday. What we’re doing is really focused on providing a company of products and service surrounded by having that conversation in a really productive way, at the right time.”
Vechery and Leahy’s product is a great first step for providing women with the preliminary knowledge of their own reproductive health. For women who are ready to take action, some are turning to a relatively new procedure that’s introducing an unprecedented cultural shift of its own: egg freezing.

The first live birth from a frozen egg was recorded in 1999, but it wasn’t until 2012, when the American Society for Reproductive Medicine took the experimental label off of egg freezing, that the procedure became readily accessible. Since the label was lifted, egg freezing has gone from something done mostly by women going through IVF and struggling with infertility to something women are proactively taking part in as a precaution. Capitalizing on this shift are shiny new clinics like Extend Fertility, where Wallace chose to have her eggs frozen.
When I visited Extend Fertility, I arrived in a nondescript high rise and ventured into a somewhat stale hallway on the fourth floor. However, once I found the door, it was a different world on the other side. The waiting room and consultation areas feel like an IKEA living room or a meeting room in a startup office. It’s far from the cold, sterile feeling often associated with doctor’s offices. When Wallace speaks of the place, she describes it as “spa-like.”

Like its exterior, Extend Fertility’s purpose is visibly and fundamentally different than that of standard fertility clinics. That’s because unlike most clinics, it’s not specifically focused on helping people overcome the disease of infertility.
“Being on the front lines of daily practice at an IVF infertility clinic, it was apparent that the setting of the traditional infertility IVF clinics was not the best way to be helping women learn about this [procedure] and choose to do it,” say Dr. Joshua Klein, the Chief Medical Officer and co-founder of Extend Fertility. “They’re just regular 21st-century women who are trying to keep their options open for the future.”
Wallace is a prime example of the type of woman that not only Extend Fertility, but an entire growing industry is beginning to cater to: the modern woman who probably wants kids, just not right now.
“There’s a sort of abstract feeling [about it all],” she says. “It’s a little bit, kind of sci-fi-esque, but I know that if this does result in a child, that October 1, 2017 will be a day of some significance.”

As much as the homey ambiance puts clients at ease, it’s still a very complex and scientific procedure women are considering when they come here. And for many, they’re not totally sure how it all works.
According to Kristen Mancinelli, Extend Fertility’s director of partnerships and education, the egg-freezing process breaks down into four phases:
The Informational Phase: When a patient expresses interest in the procedure, they’re first paired with someone from the clinic for an informational chat that will guide them through the entire journey. That’s essentially an open dialogue where they can ask all their unanswered and common questions, like, how long does it take, does it hurt, how much does it cost, etc.
If a woman wants to move forward, she’ll then come for a fertility assessment, which is basically a more thorough version of what Modern Fertility is offering at-home. This 30-minute assessment looks at two things: an Anti-Mullerian Hormone level (which gives the team a good sense of ovarian reserve, or egg supply) and a transvaginal ultrasound (which can look at the follicles on ovaries that are priming eggs for maturity in that month).
A unique element of Extend Fertility’s process is that they don’t charge for this part of the process (so long as insurance can cover the blood work required). Once the results come back, patients meet with a reproductive endocrinologist who interprets the results of the tests and really discusses whether egg-freezing is the right choice. If the results come back incredibly positive or she decides to hold off, the patient can walk away no strings attached.
The Logistical Phase: Should the patient decide to move forward, she’ll look at a calendar and schedule an egg freezing cycle. In this phase, she’ll sign all the consent forms, make the payment, and learn how to give herself the hormones shots required.
“The hardest part was that I constantly felt like I should be getting pregnant, not laying eggs.”
– Agnes Fischer
The Development Phase: The next time the patient comes in is at the start of her egg freezing cycle. This part of the process can take anywhere from eight to 11 days (it can be different for each patient). This is when women give themselves hormone injections and are required to visit the clinic roughly every other day for a quick “monitoring” visit. Here she’ll receive a blood test and an ultrasound to check in on the progress of the eggs.
When I spoke with Agnes Fischer about her own experience, she describes this phase as the hardest part. “I constantly felt like I should be getting pregnant, not laying eggs,” she tells me.
Wallace also describes this time period as physically challenging. As is commonly reported, she became incredibly bloated and described the feeling as carrying “two bunches of grapes” in her ovaries. “By the end, I had to sit delicately and I was being extremely delicate with myself,” she says.
When the eggs have grown to the right size, the doctor will tell the woman that she’s ready for what’s called a “trigger shot,” which is a different shot that she takes at the end of this phase. Then, a day and a half later, she’ll come in for her egg retrieval.
Egg Retrieval and Vitrification: The retrieval process is relatively quick, taking only 10 to 15 minutes, but it’s invasive enough that anesthesia is required. Once the patient wakes up, she’s mostly done with her part of the deal, but for the embryologists waiting on the other side of the room for the eggs, now it’s go-time.
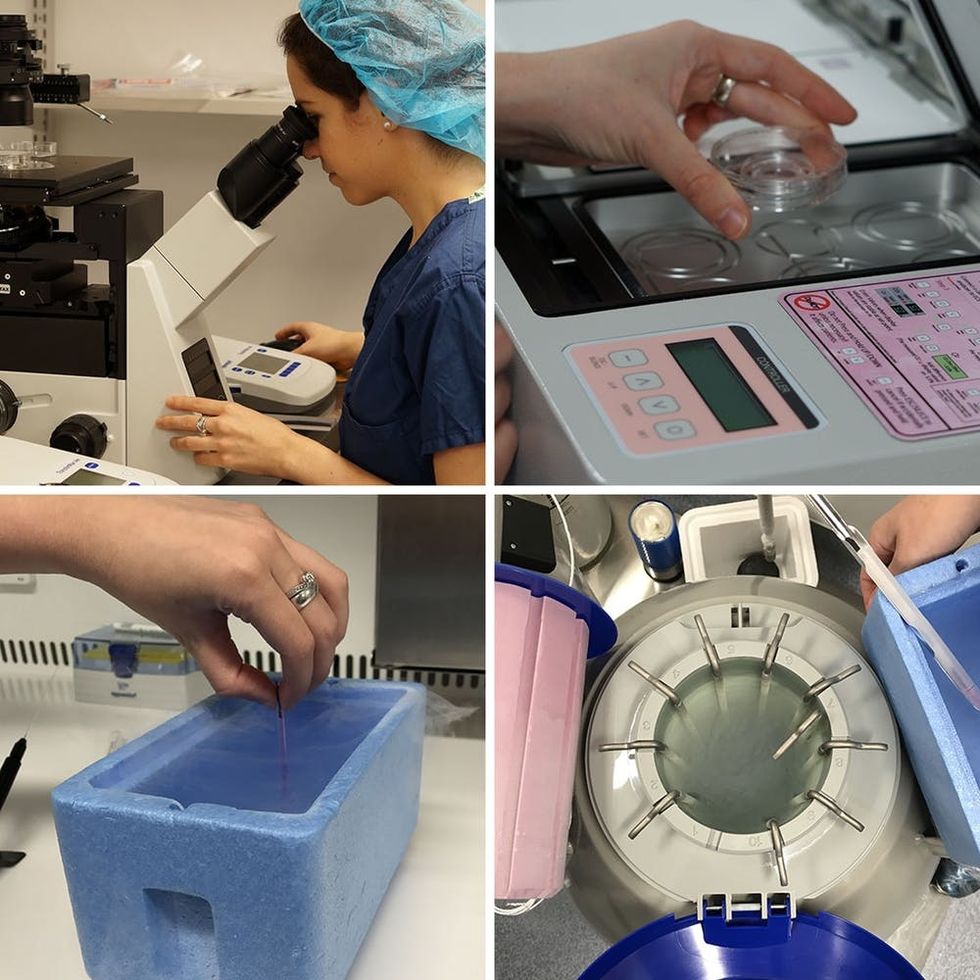
Once the eggs are extracted, they’re passed in a vial through a small window from the procedure room straight into the lab where someone like Dr. Leslie Ramirez (Extend Fertility’s embryologist who walked me through the process) will be waiting to start the vitrification — AKA, freezing — process immediately.
First, she cleans the eggs of blood and extra cells and looks for healthy eggs under a state-of-the-art microscope. Once the maximum amount of viable eggs are retrieved, they are placed in an incubator for about an hour and a half to recover from the temperature changes in their environment.
After an hour and a half in the incubator, eggs are then deposited on “straws” labeled with patient information and immediately plunged into liquid nitrogen and frozen. The combination of cryoprotectants and faster cooling (compared to the slow freezing method) reduces the opportunity for damaging ice crystals to form.
The “straws” are then capped and placed into canisters for storage. They’ll stay there for a short period of time before being sent to a long-term storage facility, where they’re held until the patient decides to use them.
For an even more detailed account of the vitrification process head here.
Impressive science aside, there’s a very obvious setback for this kind procedure: the cost. Unsurprisingly, it’s incredibly expensive. Though, depending on the circumstance and package selected, Extend Fertility’s egg freezing procedures cost up to 80 percent less than the 2017 national average, the hormones alone can cost anywhere between $2,000 to $4,000. The actual procedure costs anywhere from $4,750 to $10,000, depending on how many eggs a patient would like to try to retrieve, and long-term storage for the eggs will set patients back $350 to $450 a year. Another thing to keep in mind is that, if the frozen eggs are to be implanted at some point, that will inevitably require IVF, which will set patients back $3,000 to $5,000 more.
For women who aren’t able to write a check for somewhere in the $10,000 range (at least) but also want to wait to have babies, that poses an impossible predicament. When I asked Extend Fertility’s Dr. Klein about what can be done to help offset the shockingly high price tag, he tells me this is something they think about a lot.
To the company’s credit, it genuinely does seem like they’re doing all they can to make their services affordable. Extend Fertility patients can select a payment plan if they can’t afford the one-time payment. The clinic also offers discounts to people in certain industries, like teachers and women whose companies are corporate partners. Cancer patients get a “very special” discount.
But the reality is that, until egg freezing becomes either super normalized or a common company health benefit (tech companies like Facebook and Spotify have already started covering egg freezing), buying time is a costly investment.

Scientifically, we’ve found a way to cheat biology to a certain extent, but we’re still venturing into an unknown landscape. Are there cultural implications of older parents that we haven’t considered?
In a study conducted by the University of California, San Francisco, researchers interviewed 46 couples and 15 single women who had used in vitro fertilization to conceive their first child when the woman was 40 or older. 72 percent of women and more than half of men said they felt more emotionally prepared to parent at that point in their lives.
And when parents are better prepared, the kids benefit. A separate study looked into the relationship between older parents and their children’s test scores and found that children with older parents tended to score higher on average. Two other studies have linked the higher cognitive ability and overall well being of these children to the fact that older parents generally tend to be more psychologically mature, better equipped to roll with the punches and not freak out over minor infractions.

Even if the future does consist of genius babies and older parents, there are still a lot of unknowns when it comes to this new wave of parenting and one major question that should be considered: How will it affect the gap between generations?
If men and women are becoming parents closer to the 30-year mark, and their children are to do the same, that will inevitably cause a greater divide between generations, not only in family dynamics but also in places like the workforce where different age groups regularly work together.
There are also potentially higher biological risks that older mothers face that are less common in younger moms, though a lack of research makes this hard to be certain about. According to some studies (and a whole lot of popular wisdom), if a woman gets pregnant naturally at age 40, her fetus faces a potentially higher risk of complications, including stillbirth or genetic abnormalities such as Down’s Syndrome. (Note: These risks purportedly minimized if eggs harvested earlier in life are used, though the verdict is still out on that one.)
Despite the worries bound to accompany such a personal and cutting-edge decision, Wallace is feeling good about freezing her eggs.
“In the days following [the extraction procedure], I’ve already started to become this sort of overbearing mother,” she admits. “I’m like, Where are my eggs? I remember reaching out to the people at Extend Fertility and asking, ‘Where are they now? When are they going to long-term storage?’ And, just feeling almost concerned about where they are and are they safe and are they gonna get mixed up with other ones? I’m still feeling that way.”
The modern world of female fertility is very much still a place where logistics are being figured out, but make no mistake; advancements in this landscape are a true testament to the times. Women’s reproductive health is something the medical community is increasingly recognizing as being worthy of attention. As a result, future families may not form in the same way they used to, but it might just be for the better.
*Some names have been changed at the subject’s request
Is fertility something you actively think about? Start the conversation! Share your thoughts on the topic with us on Twitter @BritandCo.
(Extend Fertility photos via Rick Wright Photography, Design via Torii Burnett)